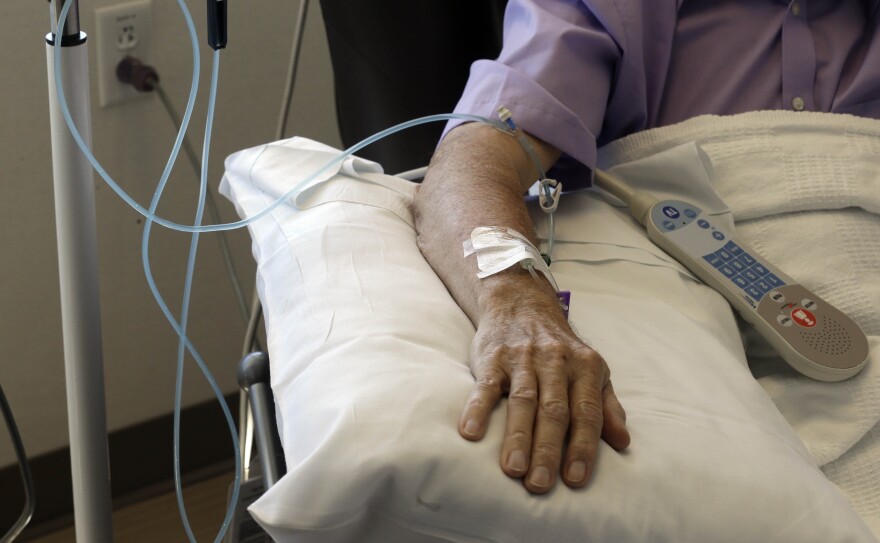
In a conversation about health, infrastructure and access to health care, River to River's Ben Kieffer spoke with two cancer experts about the common disparities between rural communities and those living in dense urban areas of the country.
Dr. George Weiner is the director of the Holden Comprehensive Cancer Center at the University of Iowa, and Dr. Robert Winn is the director and Lipman Chair in Oncology at the Virginia Commonwealth University Massey Cancer Center in Richmond, Virginia. They discussed the widening disparities in the U.S. health system, specifically disparities in cancer treatment, and how to help rural and urban communities get tested for and treat cancer.
Weiner: "There are populations in various communities that are basically underserved in many ways. They suffer from what we call 'social determinants of disease' or 'social determinants of cancer.' These are people who don't have access to care, who don't have access to healthy foods, who don't have the educational background to understand how to pursue a healthy lifestyle. What has been discovered is that there are remarkable similarities between populations in rural, underserved communities (and dense urban areas)."
"Unlike the 1960s and 70s, we can actually do things for cancer if we catch it early"Dr. Robert Winn
Winn: "I think that we sometimes forget that we live in a world of 'silos.' If you look on the south side of Chicago or some rural places in Iowa, they're more similar. The context of their poor outcomes from cancer are very similar in COVID-19. This interesting report that came out, I believe, in the Washington Post, recently, that looked at this intersection between COVID-19 and cancer. It recognized that at-risk populations like African Americans and (people in) urban, underserved areas are definitely dying more from cancer. That's actually going to be true for rural communities as well, particularly rural communities in Virginia, in Iowa and other places."
Winn: "I think many people were frightened of coming to the hospital, at least initially, and so they were either not getting the care or not getting screening. I think there's going to be a big effort of gaining people's trust and getting people to get screened. I think that's the best opportunity we have for catching cancer early. The truth of the matter is, I think as a result of having to make some tough decisions during this spike or, indeed, during the peak of this pandemic, of having put surgeries off, has actually contributed to more people not coming to the hospital and people not getting screened.
"I think as we're moving through COVID-19, the next big thing is getting cancer back on the minds of people because, unlike the 1960s and 70s, we can actually do things for cancer if we catch it early."
"Even though the distances and miles are different between the inner city and the rural challenges, the underlying challenge is the same, that traveling to get cancer care."Dr. George Weiner
Weiner: "What we have seen is a dramatic drop in people coming in to get cancer screening done, to get colonoscopies done and to get mammograms done. But we actually haven't seen that fully rebound yet.
"Our big concern is that, particularly for these underserved communities, that by the time these folks find the cancer, it's going to be more advanced and much harder to treat ... So, we haven't seen this big rush of more advanced cancers, but because we're not detecting cancers earlier, we are worried in the next six months or so that we're going to start to see an [increase] in the population of people who were struggling to get access to care."
Winn: "I was thinking about a recent paper article in, I think it's JAMA Oncology, where they said, roughly, if you look at the impact of people not being screened for the treatable cancers — the prostate, the breasts — that almost over 9 million people that should have been screened but have not been screened. That's an impressive number, and you think about that, that's just looking at prostate, breast and colon. What about lung [cancer]? I really worry about our areas, not only in Richmond, Virginia, with urban areas, but I worry about our Danville, Brunswick and in Onawa — one of the poorest areas in Iowa. I started looking at their cancer, the ability to get screened, and it's frightening."
Weiner: "They're particular challenges, actually, for those populations that are both rural and minority. In Iowa that might be some of the migrant farmers. In Virginia, that might be some of the African American and rural poor [communities]. Not only do they have difficulty in the distance, but they have all the other challenges that are also experienced in the city: food and food deserts."
"Infrastructure in our country is going to be something that we're going to use more extensively in cancer diagnosis and treatment."Dr. Robert Winn
Winn: "I have to readily admit when, initially, I was thinking about food deserts, I had that in my mind of some areas on the south side Chicago. Meaning, for example, there was not access to fresh fruits or vegetables. There wasn't really even access to fresh meats. It turns out that I was wrong. If you look at places in Virginia, Ohio, and even in Iowa, rural areas also, just like the south side and west sides of Chicago, have areas where they don't have access to all that fresh [food]."
Weiner: "We do have access to the healthy foods, that Rob talked about, but are just very limited in both the inner city, some of the rural poor community and the rural poor communities. Getting the healthy foods is difficult; They're more expensive. People have to travel further to get transportation — another very interesting parallel. Even though the distances and miles are different between the inner city and the rural challenges, the underlying challenge is the same, that traveling to get cancer care. Traveling to get cancer screening is an incredible challenge for folks both in the inner city where they might have to take three buses and transfers and spend hours doing it, versus a rural community where there's just no way to get to the medical center.
"This has limited both communities from getting screening."
"Both urban underserved communities and rural populations have an interesting issue with science, medicine and trust."Dr. Robert Winn
Winn: "Everyone talks about social determinants of health as if it's a hashtag, right? They talk about food insecurity and housing insecurity. But the one thing I think we all can agree on is that, as health systems, we certainly can do things about transportation, and we should be advocates for broadband.
"I think the American Cancer Society had put out over something like 4 million people a year wind up having poor outcomes simply because they couldn't get care. Transportation really is a social determinant of health that's usually connected to other things. So if you don't have good traveling or good transportation, you probably don't have some of these other things as well. I think it's high time that as health systems, and as people who are really committed to public health, we pay more attention to transportation, particularly urban, underserved and rural areas, because I think that if we can get you to point A to B, we can do something. If we can't even get you into our doors, we can't screen you and we can't do a whole lot of things. As we get through COVID-19, we're gonna have to think about 'how do we get to people?' Probably that's going to be broadband, telehealth and mobile health. But how do we actually also get this transportation gain fixed so that we can get people back and forth to get their health? Infrastructure in our country is going to be something that we're going to use more extensively in cancer diagnosis and treatment."

Weiner: "We have learned some lessons. This is a tiny silver lining in the pandemic and learning how to use telehealth. So we need to learn our lessons and utilize this new technology to the greatest degree available."
Winn: "I have to say that both our urban underserved and rural populations also have been susceptible to misinformation, disinformation and interestingly enough, both in a very similar manner. We're starting to see issues of trust, and I never, probably when I started my career in science and started my career as a physician, would have actually focused on this context of trust. But it's becoming — it's risen to a head now that I can no longer ignore that both urban, underserved communities and rural populations have an interesting issue with science, medicine and trust. I think we're going to have to start rolling up our sleeves, putting on our thinking caps, and figuring out how we as institutional academic centers, and health systems, can not just regain the trust, but figure out how we can even improve our own trustworthiness."
"It's hard enough just to take care of cancer, but it's even harder competing against 'Doctor TikTok.'"Dr. Robert Winn
Weiner: "Well, I think that the challenge is that people have difficulty identifying sources of truth. The democratization of information that has come with the internet has had many wonderful positives, but one of the real challenges is that it makes it difficult for people to really figure out what to pay attention to. Part of what we need to do is to continue to speak about the truth, but to do it in a way that is culturally sensitive to the different communities.
"This is one area where the language you use in an inner-city may actually be different from the language you would use in a rural, underserved community, but the message has to be the same, which is to really help point people towards the facts so that they can put this information, that they're also being bombarded with, in perspective."
Winn: "It's hard enough just to take care of cancer, but it's even harder competing against 'Doctor TikTok.' There are days where you're essentially saying you really do need to get screened, and someone saying, 'well, you don't need to get screened. I just saw this on TikTok,' and it is difficult and becoming increasingly more difficult to manage and to navigate healthcare.
"Now I have to be honest with you, some of this probably is our own fault. While we have been creating scientific miracles, we have not always been connecting with communities in a way to ensure that they are understanding the science, or the understanding in plain simple terms, what's going on. Think like a wise man, but communicate in the language of the people. We need to be able to communicate in a more effective way, and so I think people sometimes get disenchanted and are looking and searching for information, but it's almost like that one's all looking for information in all the wrong places."
"How do we take the advances we have and make sure that people in these underserved communities can benefit from them?"Dr. George Weiner
Weiner: "This is actually a really important area of cancer research right now. It's great for us to make these discoveries and develop new treatments, but if they don't get out to help people, we haven't served our purpose. So a very important aspect of research is health delivery, research, and communication. How do we take the advances we have and make sure that people in these underserved communities can benefit from them?"
Winn: "I think that, you know, this is really something that's been with us for a very long time. Cesar Chavez and Martin Luther King got together, recognize that their struggles were more similar than different. I think in a similar way, rural communities, places in Iowa, places in Virginia, share commonality poor outcomes of cancer and poor outcomes of health just like on the south side of Chicago or in the Bronx of New York. We have to fix that. I think we have to get beyond race and recognize that where you are placed in space really matters, and I think by focusing on broadband and getting more equity, building infrastructures, focusing on transportation and just good communication, is where we can at least make a dent."
Weiner: "Well, we can learn from each other. One of my heroes, and Rob's as well, is a surgeon, Harold Freeman, who recognized this problem and developed a patient navigation system to help inner-city, underserved people navigate the complexity of the medical center. We need to do that in rural communities as well. We need to work together, figure out what works, figure out how we can learn lessons, take lessons learned in each community, and apply them to all people who need our services."
This conversation originally aired on River to River on October 12, 2021.